Disclaimer: This article is for educational purposes only and is not a substitute for professional medical advice. Always consult a qualified healthcare provider for concerns about your health.
Discovering a bump, spot, or unusual skin change in the genital area can feel stressful. However, dermatologists and sexual health specialists note that genital skin variations are common and often harmless. Understanding the possible causes can help you respond calmly and seek medical care when necessary.
Because the genital area is sensitive and prone to friction, moisture, and hormonal influences, it is especially vulnerable to irritation and benign skin conditions. At the same time, some infections or medical conditions may require evaluation and treatment. Knowing the difference is important for protecting your health.
Common Benign Causes of Genital Bumps
1. Folliculitis
Folliculitis occurs when hair follicles become inflamed, often due to shaving, waxing, tight clothing, or bacterial exposure. Medical sources such as dermatology associations note that this condition is common anywhere hair grows, including the pubic area.
Typical signs include:
-
Small red or white bumps
-
Mild itching or tenderness
-
Occasional pus-filled spots
What helps:
Keeping the area clean, wearing loose clothing, and avoiding shaving until healed can reduce irritation. Warm compresses may support healing. If symptoms worsen, spread, or do not improve within several days, a clinician may recommend topical or oral treatment.
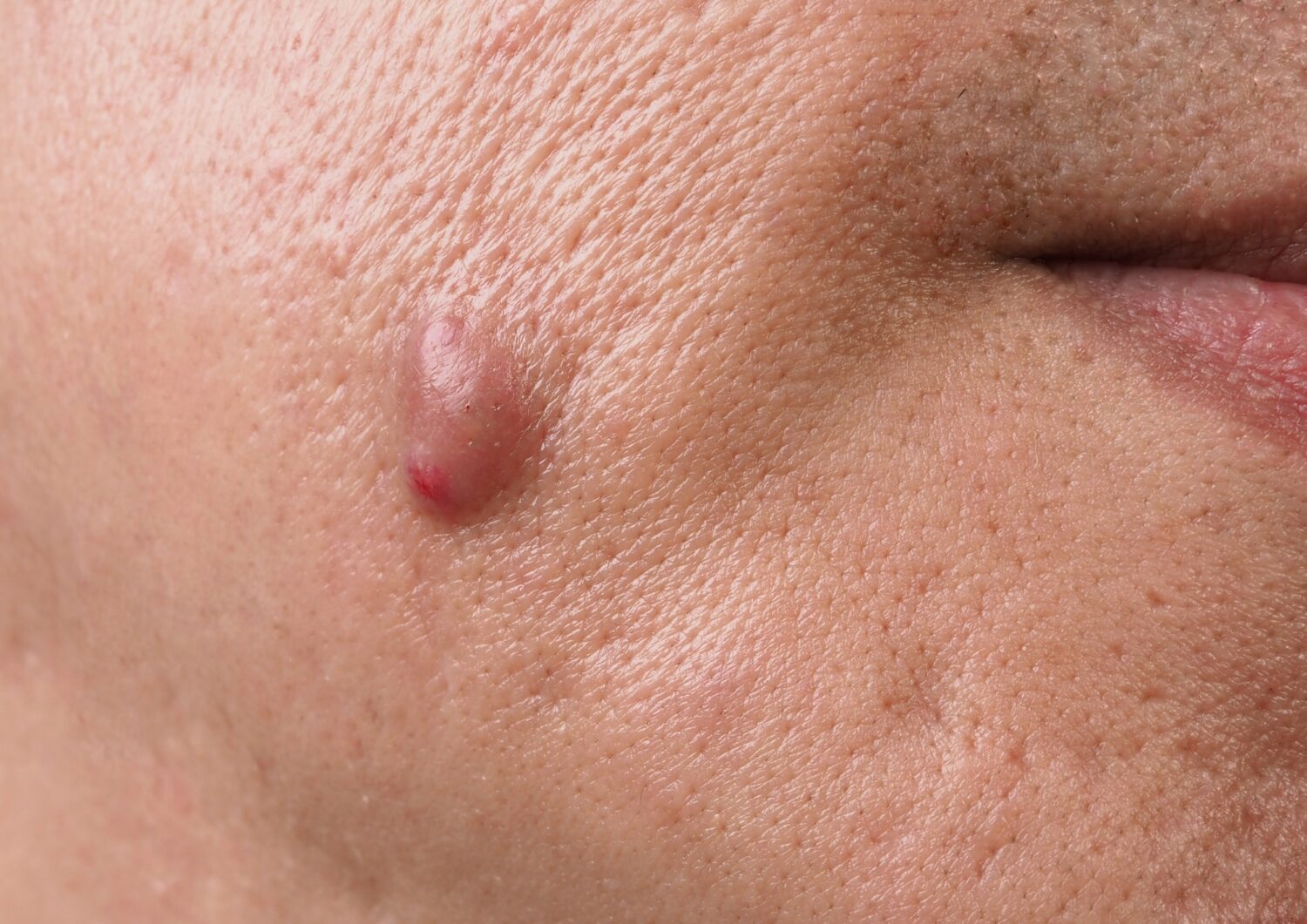
2. Sebaceous or Epidermoid Cysts
Sebaceous or epidermoid cysts form when skin glands or follicles become blocked. They are usually benign and can appear anywhere on the body, including the genital region.
Typical signs include:
-
Smooth, rounded lump under the skin
-
Flesh-colored or slightly yellow appearance
-
Usually painless unless inflamed or infected
What helps:
Most cysts do not require treatment. Medical evaluation is recommended if a cyst becomes painful, grows rapidly, or shows signs of infection such as redness, warmth, or drainage.
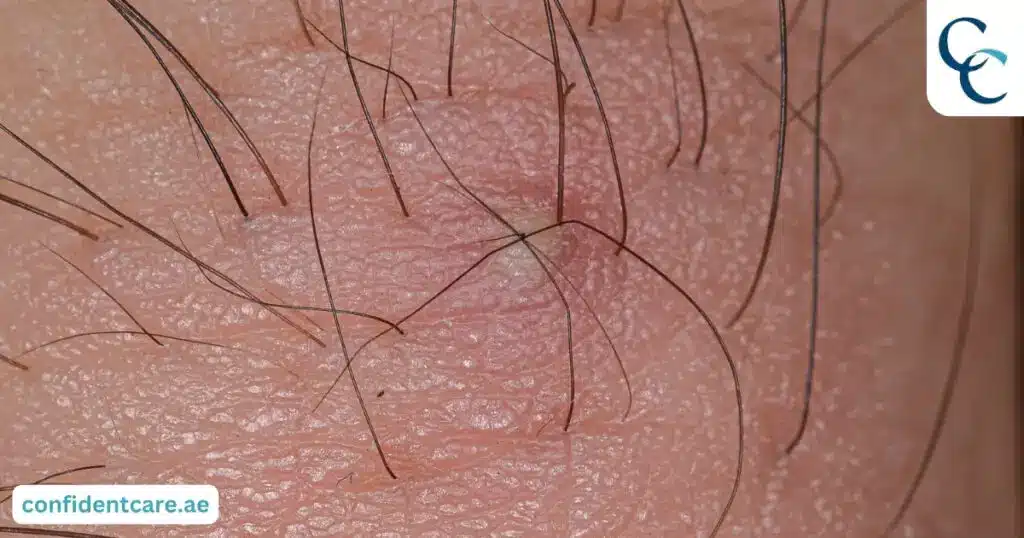
3. Ingrown Hairs
Ingrown hairs develop when shaved or waxed hair curls back into the skin. They are particularly common in the pubic region.
Typical signs include:
-
Small red bumps
-
Mild discomfort or itching
-
Visible hair trapped beneath the skin
What helps:
Avoid picking or squeezing the bump, as this can increase infection risk. Gentle exfoliation and pausing hair removal can allow the hair to grow out naturally.
4. Fordyce Spots
Fordyce spots are visible sebaceous glands that appear as small pale bumps on genital skin. Medical literature describes them as a normal anatomical variation rather than a disease.
Typical signs include:
-
Tiny white, yellow, or skin-colored dots
-
No pain, itching, or discharge
-
Often present long term
What helps:
No treatment is necessary. If unsure whether bumps are Fordyce spots, a clinician can confirm the diagnosis during a routine exam.
Conditions That Require Medical Evaluation
While many genital bumps are harmless, some conditions should be assessed by a healthcare professional for accurate diagnosis and treatment.
1. Genital Warts
Genital warts are caused by certain strains of human papillomavirus (HPV). Public health agencies identify HPV as one of the most common sexually transmitted infections worldwide.
Typical signs include:
-
Flesh-colored or gray growths
-
Smooth or cauliflower-like texture
-
Often painless but may itch or bleed
Why medical care matters:
A clinician can confirm the diagnosis and discuss treatment options such as topical medications or minor procedures. Vaccination against HPV can reduce the risk of infection.
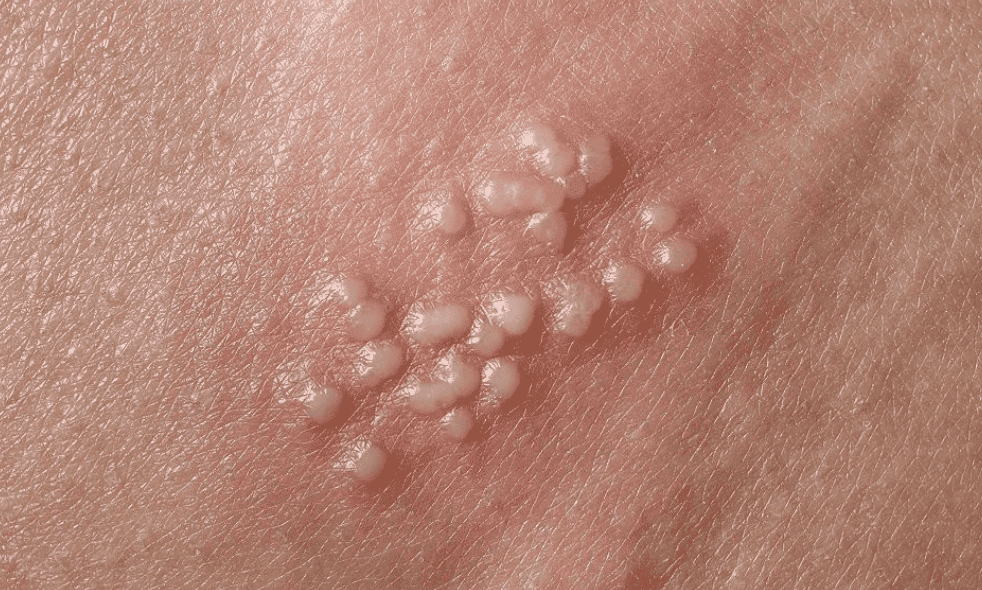
2. Herpes Simplex Virus (HSV)
Genital herpes is caused by the herpes simplex virus. Health authorities emphasize that many people with HSV experience mild or infrequent symptoms, but outbreaks can still occur.
Typical signs include:
-
Painful blisters or sores
-
Tingling or burning sensation before lesions appear
-
Flu-like symptoms during initial infection
Why medical care matters:
Antiviral medications can reduce outbreak severity and lower transmission risk. Early diagnosis also helps individuals understand how to manage symptoms and protect partners.
3. Molluscum Contagiosum
Molluscum contagiosum is a viral skin infection that spreads through direct contact. It can affect adults and children and may appear in the genital region in sexually active individuals.
Typical signs include:
-
Small, firm, dome-shaped bumps
-
Central indentation
-
Usually painless
Why medical care matters:
The infection often resolves naturally but may require treatment if lesions spread or cause discomfort.
4. Skin Conditions and Dermatitis
Chronic skin conditions such as eczema, psoriasis, or contact dermatitis can also appear in the genital area.
Typical signs include:
-
Red, flaky, or inflamed skin
-
Itching or burning
-
Recurrent irritation after exposure to soaps, fabrics, or products
Why medical care matters:
A healthcare provider can identify triggers and recommend treatments such as medicated creams or lifestyle adjustments.
When to See a Healthcare Provider
Medical professionals generally recommend evaluation if you notice:
-
Painful or rapidly growing bumps
-
Sores that do not heal within two weeks
-
Fever or flu-like symptoms
-
Unusual discharge or bleeding
-
Recurrent lesions
Prompt evaluation helps ensure accurate diagnosis and prevents unnecessary anxiety.
Protecting Genital Skin Health
Healthcare experts often suggest several simple practices to support genital skin health:
-
Maintain good hygiene without over-washing
-
Choose breathable, loose-fitting clothing
-
Avoid harsh soaps or fragranced products
-
Use protection during sexual activity
-
Seek routine health screenings when appropriate
These steps can reduce irritation, infection risk, and unnecessary skin inflammation.
Final Thoughts
Genital bumps and skin changes are common and often harmless, but they should never be ignored. Understanding potential causes—from simple irritation to infections—empowers individuals to make informed decisions about their health.
If you notice persistent, painful, or unusual changes, consulting a qualified healthcare provider is the safest course of action. Early evaluation supports both physical wellbeing and emotional reassurance, ensuring that minor concerns remain manageable and serious conditions are addressed promptly.
